Local
A year after surviving COVID, business is flourishing
Darryl and Joe Ciarlante-Zuber on facing death — and the birth of Rehoboth’s Square One

Last year, Darryl Ciarlante-Zuber nearly died from the novel coronavirus while his husband, Joe, sat in quarantine.
After 40 days of intensive care at Beebe Medical Foundation and a year of support from their friends and the community, the duo have since opened a second restaurant and are thriving.
Joe, who was in Mexico, received a call on March 28, 2020, from his husband complaining that he was having difficulty breathing. After instructions from his doctor, Darryl packed for a supposed three-night stay at the emergency room.
“It was like [my doctor] really wants me to go to the ER, and I don’t really feel that sick,” Darryl said. “I said, ‘I’m just out of breath, up and down steps, but other than that, I really didn’t feel sick.’”
Three nights turned into a call from clergy, asking Joe if Darryl would like some prayers. The second call Joe received was from a doctor in the ICU.
“They said Darryl has 30 minutes to live and is severely ill,” Joe said. “[They said] his lungs are nearly totally collapsed and filled with stuff, and we want to put him on a ventilator.”
Joe’s impromptu and urgent flight from Mexico back to Rehoboth was filled with anxiety, especially since not much was known about the coronavirus that early in the pandemic.
“Is he going to be alive? Is he going to be dead? It’s COVID, what is this COVID thing?” Joe said. “I was on a plane, and I was one of the only ones with a mask. The reason I had a mask is because my friend who drove me to the airport had a mask from his maid and said, ‘Here, use this.’ It was a whirlwind experience.”
Darryl spent 23 days on life support, while the recommended time for a ventilator is a maximum of six days.
“The doctors told [Joe], ‘We just don’t know how he’s going to come out,’” Darryl said. “But at the time, the doctor said, ‘Well, that seems like it’s the only solution at this point.’ So he pushed it for Joe until the 23rd day.”
Prolonged time on a ventilator can prove dangerous, Joe said, as he was warned about potential negative effects on Darryl’s brain.
“They routinely told me that he would have brain damage and he may or may not be the same person that I knew,” Joe said. “And I said, ‘I’m OK with that.’ When I took my vows, we said that we would be partners forever, husbands forever. If he has brain damage, I’m the one that’s going to deal with it, nobody else.”
Darryl was the third patient in the Beebe ICU to be diagnosed with COVID-19. While in the ICU, Darryl’s white blood cell count fell to only nine, according to Joe.
“They basically said to me, ‘Look, it’s been 20-some days. There’s no recovery, you need to let it go,’” Joe said. “And by some goofy chance, his [white blood cell] numbers jumped from 12 to 25,000, and they went up to 50,000. They have to be 80,000 to take the trach out, and Monday morning, they were at 83,000.”
Darryl said he does not remember much after being led into the ICU from the hospital waiting room.
“I had Joe on FaceTime the whole time just to make sure I was getting there OK,” Darryl said. “I was like, ‘OK, they’re probably going to take me in soon, I’m going to probably lose reception in the hospital and I can’t call but I’ll call you when I can.’ And I just remember hanging up. They took me out of [the entrance] and that’s all I remember after that.”
After 23 up-and-down days on life support, Joe said the Beebe team members spent 40 days dedicated to Darryl’s treatment and that he was constantly given updates, since quarantine protocols were in effect.
“Darryl’s nurses in the ICU were my link to being with him when I couldn’t actually visit,” Joe wrote in a Feb. 9, 2021 essay for the Cape Gazette. “They would assure me that he could hear my voice, even though he made no response. They would tell me that sometimes Darryl would move his feet in reaction to certain things I said to him.”
While Darryl received treatment, Joe updated family and friends through Facebook.
“If I didn’t post something by 11 in the morning, people were calling, ‘What’s happened, how come? Is everything OK?’” Joe said. “Sometimes you just didn’t hear and I didn’t have any information from the doctors or the nurse, they were full, and they had these patients.”
Darryl’s 40 days of treatment finished with physical therapy and rehab.
“I had no movement, I had to relearn walking,” Darryl said. “I had lost all my strength in my arms and so the first two weeks was to try to get me, at least somewhat capable, to move forward to the rehab center.”
Darryl also said that Joe kept a lot of information from him so as not to worry him or worsen his condition, including the severity of the coronavirus in the United States.
“One of the things he had asked me when he was in the hospital, he said, ‘Why aren’t you working?’ and I said, ‘Darryl, everything’s closed,’ and he looked very confused,” Joe said. “You know Nicola Pizza? They never close, never. I said to Darryl, ‘Nicola’s is closed, because of the pandemic.’ He said, ‘Nicola’s is closed?’ [Darryl] got really sad in his eyes and he said, ‘It’s bad, isn’t it?’ So I said, ‘But everything’s getting better, so don’t worry about it, just get yourself better.’”
Darryl and Joe opened Diego’s Bar & Nightclub in 2018, the name a nod to Darryl’s nickname. The bar closed in 2020 like all other businesses due to the pandemic, however the duo did not let Darryl’s condition or the lockdown procedures keep them down.
“Some of the positives about Diego’s is, we were able to create a beach. We took over some of the parking lot and created a beach atmosphere, tables and chairs and umbrellas and transporting nine tons of sand, and socially distanced all the tables,” Joe said. “It really made a lot of the customers feel even more safe, especially being outside.”
Darryl was unable to return to his typical work day, as pinched nerves were causing pain from standing for too long.
“That’s kind of an emotional thing, because you’re used to doing something then all of a sudden, you can’t,” Joe said. “Everybody looks at him and says to him, ‘You shouldn’t be here,’ and he says, ‘I know,’ and they said, ‘Your charts, you are truly a miracle.’”
Before the pandemic, Joe and Darryl made several attempts to open a new restaurant location. In February 2021, the timing worked out and the two opened Square One Grill.
“Fortunately, we found our head chef in December and we just talked about opening up by the end of January, to get it in time for President’s Day weekend,” Darryl said.
Square One general manager Trish Carlin said the restaurant began with experimental takeout dishes for the community, since lockdown efforts kept indoor seating to 50 percent capacity and the team decided to keep the dining room closed.
“[Darryl and Joe] just reached out to so many people that they knew and they set up [takeout] for a group of days, where people could order food and pick it up for free,” Carlin said. “They would want comments on it, how did this work? What did you think about that? They got a lot of feedback.”
Diego’s dance floor opened in late May and the dining room in Square One is also open for customers. Darryl, Joe and Carlin all discussed the community’s positive efforts and support in keeping the businesses alive.
“I felt like the community was waiting for Joe and Darryl to finally be able to do this. And maybe that was part of their motivation,” Carlin said. “I was never worried, honestly, that it wouldn’t work, because it’s them. I think the community really backs them. They really, really love Joe and Darryl and they follow them wherever they go. They want them to be successful and it’s a wonderful thing to see.”

District of Columbia
D.C. Pride flag raising ceremony set for June 1
Mayor, council members to participate
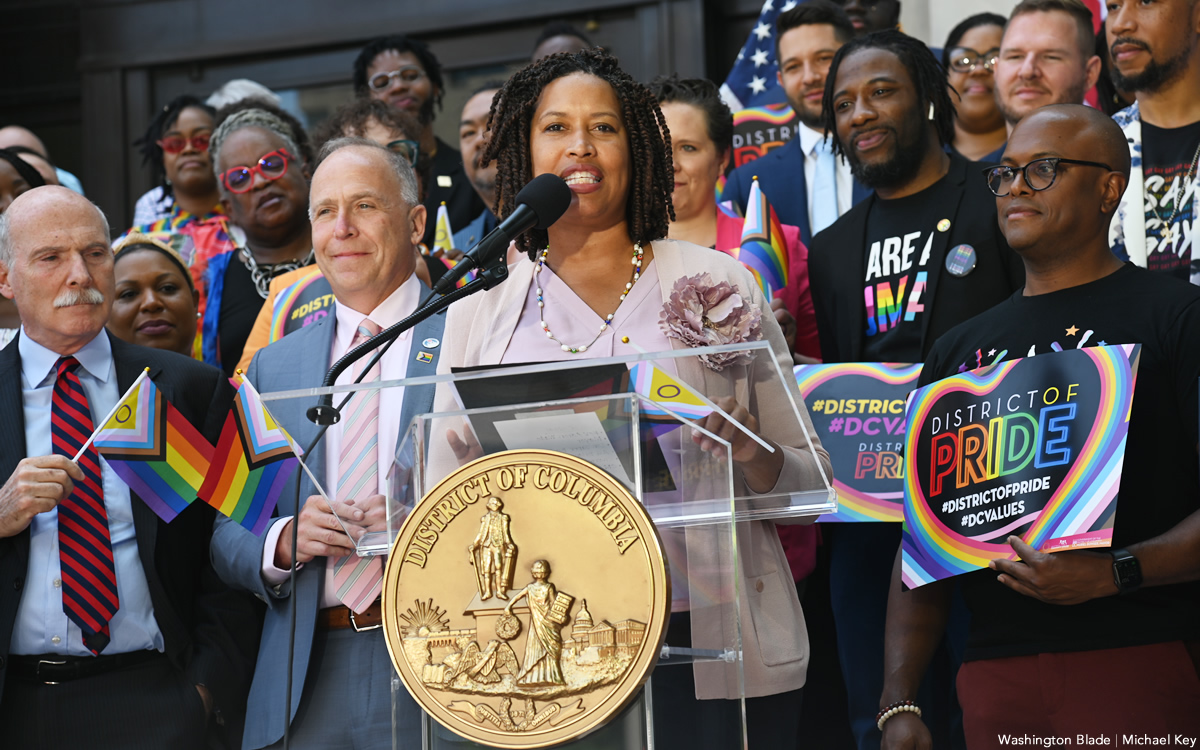
D.C. Mayor Muriel Bowser’s Office of LGBTQ Affairs is inviting the LGBTQ community and friends to attend the city’s annual Pride flag raising ceremony scheduled for 4 p.m. Monday, June 1, outside the John Wilson Building that serves as the D.C. City Hall.
Like in prior years, members of the D.C. Council and officials with the Office of LGBTQ Affairs were expected to join Bowser in delivering remarks on the front entrance steps at the Wilson Building before raising the Pride flag atop one of the tall flagpoles next to the building’s entrance.
Gaby Vincent, a spokesperson for the LGBTQ Affairs Office, said attendees of the flag raising ceremony will be invited to attend a reception immediately following the ceremony in the main lobby of the Wilson Building, which is located on Pennsylvania Avenue at 14th Street, N.W.
She said the reception will feature a DJ, dancing, and refreshments provided by the D.C. LGBTQ bar and café Spark Social House.
Vincent said the flag raising event will also mark the 20th anniversary of the opening of the D.C. Mayor’s Office of LGBTQ Affairs.
In its official announcement of the flag raising event the LGBTQ Affairs Office also announced it is hosting the 7th annual District of Pride Showcase event to be held Friday, June 17, at 7 p.m. at the Lincoln Theater.
The announcement says LGBTQ community members, families, and allies are also invited to walk with Bowser in the Capital Pride Parade scheduled for Saturday, June 20. It says the mayor’s parade contingent will assemble at 2 p.m. at the parade’s starting location at 14th and U Streets, N.W.
“As we also celebrate the 20th anniversary of the Mayor’s Office of LGBTQ Affairs, we invite residents, community members, families and allies to join us throughout June for moments of pride, connection, visibility, and joy,” the announcement says.
District of Columbia
‘Queer Love’ campaign launched to address domestic violence
D.C. event set for LGBTQ+ Domestic Violence Awareness Day on May 28

The D.C.-based Wanda Alston Foundation, which provides housing and support services for homeless LGBTQ youth, announced earlier this month that it has joined partner organizations to launch a Queer Love Shouldn’t Hurt campaign aimed at addressing domestic violence within the LGBTQ community.
In a May 18 statement, the Alston Foundation said the campaign involves a public awareness initiative leading up to LGBTQ+ Domestic Violence Awareness Day scheduled for May 28.
“Domestic and family violence in LGBTQ+ communities is real and too often invisible,” Cesar Toledo, the Alston Foundation’s executive director, said in the statement. “As a community, we do not talk about it enough, and that silence can leave survivors feeling isolated and alone,” he said. “We must break that silence.”
He added that culturally competent care for those impacted by domestic violence is available through a newly launched website, queerlove.org, “where people can safely access vital resources, educational toolkits, and support networks they need on their healing journey.”
The website announces one of the project’s first events, a Queer Love Community Social, was scheduled for Thursday, May 28, from 6-8 p.m. at the D.C. LGBTQ+ Community Center at 1827 Wiltberger St., N.W.
“Join us this LGBT+ Domestic Violence Awareness Day for a community social dedicated to visibility and survivor resilience,” the website statement says. “Let’s gather to strengthen our bonds, honor the path to healing, and share free resources,” it says of the May 28 event.
The website also announces a June 1 workshop called Empowering Survivors of LGBTQ+ Intimate Partner Violence, which it says will be presented by Jesse Wedell, an official with the D.C. LGBT+ Counseling Collaborative. The website provides an online form to register for the workshop upon which its location would be disclosed.
It identifies the partner organizations working with the Alston Foundation on the Queer Love Public Awareness Campaign as the LGBT+ Counseling Collaborative, Whitman-Walker Health, the D.C. LGBTQ+ Community Center, and Equality Chamber.
The resources and information provided by the project can be accessed at www.queerlove.org.
District of Columbia
Man accused of threatening to shoot D.C. bar employee after making anti-gay slurs
May 24 incident took place near Black Pride events on U Street

D.C. police on Sunday, May 24, at around 4:20 p.m. arrested a Maryland man for allegedly threatening to shoot an employee while using anti-gay slurs at Ben’s Next Door restaurant and bar at 1211 U St., N.W.
According to a statement released by police and a police incident report, the arrested man, identified as Delonte Fraley, 32, of Accokeek, Md., made the threats after the employee told a bartender not to serve the man alcohol.
“The suspect overheard the employee and threatened to shoot the employee and used homophobic slurs against the employee,” the police statement says. “When the employee left the restaurant for the day, the suspect was standing near the employee’s vehicle,” it says.
“The employee returned to the restaurant and called the police,” the statement continues. “The suspect was apprehended by responding officers,” it says.
The police statement says the arresting officers charged Fraley with Felony Threats (Hate/Bias).
D.C. Superior Court records show prosecutors with the Office of the U.S. Attorney for D.C., which prosecutes D.C. criminal cases, escalated the charge to Threatening to Injure or Kidnap a Person (Bias-Related Hate Crime).
The incident occurred during Memorial Day weekend when thousands of visitors and D.C. area LGBTQ advocates and supporters were attending D.C. Black Pride events held in locations across the city, including Black Pride parties hosted by LGBTQ bars in the U Street entertainment area near Ben’s Next Door.
Among the nearby LGBTQ bars hosting D.C. Black Pride events were Nellie’s Sports Bar and Thurst Lounge. Ben’s Next Door is located next to the popular longtime U Street eatery Ben’s Chili Bowl.
Court records show that Judge Robert R. Rigsby at a May 25 presentment hearing released Fraley on personal recognizance with a stay-away order — the details of which were not publicly disclosed pending a June 4 preliminary hearing.
A more detailed arrest affidavit filed in court by D.C. police says Fraley allegedly confronted the employee at Ben’s Next Door with anti-gay slurs on the day prior to his arrest.
“The complainant told the defendant that because he used homophobic slurs towards himself previously on May 23, 2026, and his hostess, as well as making threats to the complainant and calling him a faggot, he was unable to stay in the establishment,” the affidavit states.
It adds, “The defendant became irate stating, ‘I know where your Tesla is at. See me outside faggot, I will slap your ass’ and ‘I will shoot your ass.’” The affidavit says the complainant confirmed to police the Tesla referred to by Fraley was his vehicle. It says as the victim walked toward his car after getting off work, he saw Fraley standing directly in front of the car.
“The complainant stated he felt unsafe while the defendant was standing in front of his vehicle because he felt the defendant was capable of carrying out those threats,” says the affidavit. It says the victim then decided to return to the restaurant and call police without the defendant having seen him.
“The defendant was placed under arrest for Felony Threats Hate/Bias and was transported to the Third District Station for processing,” the affidavit concludes.
It couldn’t immediately be determined whether the victim identifies as LGBTQ or whether any of the Ben’s Next Door patrons had been involved with D.C. Black Pride.
“Established in 2008, Ben’s Next Door is a family-owned and operated restaurant and bar on U Street, Northwest in Washington, D.C.,” a statement on its website says. “As a Black-owned establishment, it’s our goal to deliver a warm, welcoming, familiar, and communal vibe to all guests,” the statement says.
-

 2026 Midterm Elections3 days ago
2026 Midterm Elections3 days agoBree Fram’s congressional campaign ends but her fight continues
-

 Celebrity News3 days ago
Celebrity News3 days agoPeppermint made her mark on ‘Drag Race.’ Now, her advocacy is front and center
-

 Opinions3 days ago
Opinions3 days agoWhy this Black Pride, I ranked Janeese Lewis George #1 for D.C. mayor
-

 a&e features3 days ago
a&e features3 days agoFrom Media Matters to massive queer ragers: the rise of Tara Dikhof


















