District of Columbia
Recovery at the Triangle Club
Coming together as a group to fight a common addiction

On Sunday, between the Dupont Italian Kitchen, where the tables are filled with the boozy brunches of the kickball gays, and Mikko, where a young couple is celebrating their anniversary with some Champagne, the door to a row-house opens, and all at once, a crowd pours forth onto the stairs. Only the stairs keep on filling. These folks aren’t leaving. They’ve only left the building to come to the stairs, just to chat. It’s as though 100 people all decided to go for a smoke out front, all at the same time. But if you ask them why they’re there, you’ll get only the vaguest of answers. “We’re just coming from a meeting,” one will say. “It’s a clubhouse,” says another.
There are good reasons for this vagueness. The Triangle Club is a center for queer folk to attend recovery meetings: Overeaters Anonymous, Alcoholics Anonymous, Crystal Meth Anonymous, Sexual Compulsives Anonymous. It’s part of the very mission of these groups to protect the privacy of their members. But these groups also want those in the queer community who need the support to know that they’re there. And so the folks at the Triangle Club were kind enough to welcome the Blade into their space for a few meetings, to see how things worked and shed some light on what they’re all about.
The Club had its kickoff meeting in 1988, during the AIDS crisis. Churches weren’t particularly enthusiastic about hosting gay recovery meetings in their back rooms. And so the Club sought to provide a safe place for those meetings to take place. At the time of the club’s founding, it was estimated that gays and lesbians were twice as likely to report problems with alcohol abuse than heterosexuals. One would hope that things might have changed in the intervening years. But according to a government report released this summer, that figure has barely improved. (The government report did not collect any statistics on transgender people.)
Of course there is no single reason queer people develop problems with drugs and alcohol. But one in particular struck me, especially as a reason I heard coming from a lot of the younger folk at the Triangle Club. “I thought meth was a prerequisite for going out,” said one. “I thought that’s what you did.” Another said, “I drank to find community. And then I drank to numb myself when I didn’t find it in the gay community.” Again and again, I heard stories about turning to drugs and alcohol as a way of finding connection, and as a way of coping with the failure to find connection.

And so while I heard a lot of gratitude for the role the meetings at the Triangle Club played in people’s recovery, I also heard a lot of gratitude for the community of the Triangle Club itself. It wasn’t just that the Club helped people turn away from an unhealthy way of solving their problems. It’s that it gave them what they were really looking for in the first place: a community they could call their own.
Improbably, as I left a meeting of Crystal Meth Anonymous, I found myself wishing to be an addict in recovery. To have a place to share things that would go unsaid among friends and family, let alone therapists. To take part, week after week, in one another’s mission for a more fulfilling life. To be present for the absolute raucousness, as when one gentleman described living on meth as “wearing a fur coat into a swimming pool,” and then “turning the wave-machine on.” To hear the applause that only someone four days sober could receive. But what kind of destructive, life-threatening wish was I making? I couldn’t possibly be serious.
Many of us in the queer community are exhausted by drinking, if not drugging, our way into it. That exhaustion might not rise to the level of addiction, but this has the perverse consequence of not driving us to seek alternative forms of belonging. One of the men I interviewed kept talking of the “sober community,” and my ears perked up. Perhaps there was a broader community of folks, of which those in recovery were only a part, that wasn’t centered around substance use.
“The sober community absolutely extends beyond the Triangle Club,” he told me. “There are a bunch of other gay meetings that go on.” This wasn’t exactly what I hoped to hear. What a sorry state we’re in, I couldn’t help but feel that to be part of the sober community was to be in recovery. As though the community of substance use were so mandatory that it had to drive you to your own personal edge in order for you to find community in sobriety.
The Triangle Club should not be overly romanticized, and they’d be the first to tell you. People talked of trying to find fellowship at the club in the past, and not necessarily succeeding. Being one of two Black people in the room, only for the other to drop out of the program. Or of the demands of service, dragging yourself out late Friday night to chair a meeting, or sponsoring someone for the first time and being scared that you aren’t the right one to advise them. But I think it’s a testament to the space that these things could be said in the space. The meetings aren’t a place of mandatory optimism, but honest experience. And what good is a meeting for sharing honest experience if you can’t share your negative experiences too?
I had hoped, as part of this feature, to attend a meeting of Sexual Compulsives Anonymous. The two meetings I appealed to were kind enough to hold a vote on whether they would open their doors—but in the end they opted to remain private. One gentleman from the meetings volunteered to share a little of what these meetings were all about. Recovery meetings in general depend on coming together as a group to fight a common addiction. But “S” meetings, as the gentleman described them, can’t take “coming together” lightly, nor a “common addiction” lightly.
To begin with, sexual addiction is not as straightforwardly defined as addiction to drugs or alcohol. What sobriety is for one person is not what sobriety is for another. One person might be trying to curtail a masturbation habit. But for others? “That simply isn’t an option,” the gentleman said. And unlike recovery meetings for substances, which can ban substances from the room, the same can’t as easily be said for “S” meetings. We’re sexual beings, and so inevitably, to bring yourself into a room is to bring sexuality along with it. The recovery meetings at the Triangle Club usually end with the group joining hands to say the serenity prayer. But this can’t be a given at “S” meetings, where joining hands might be violating someone’s boundary.
With the pandemic waning, most recovery meetings have slowly started to transition away from video format back to in-person. But “S” meetings have been more reluctant to do so, and most have stuck with a hybrid format. One veteran of Al-Anon voiced his relief at coming back to the rooms. “You can’t hug a square!” I suspect that’s the very reason “S” meetings have been slow to return.
Part of my disappointment in not attending the “S” meetings was how central they seemed to be to a queer recovery organization. Substance abuse might disproportionately affect the queer community, but it is the addicts who are queer, not the addictions. If the addiction is to love or sex, however, the addiction itself is inextricably queer. Aren’t the “S” meetings the heart, in a sense, of the Triangle Club? But a conversation with a gentleman from Alcoholics Anonymous had me rethinking this. “[Accepting you’re an alcoholic,] it’s similar to coming out as gay,” he said. “There are people out there who view it as a moral failing, but it’s just part of who I am.”
The experience of coming out is so central to being queer. How could coming out as an addict have nothing whatsoever to do with it? The same story of a newfound, authentic life was as common to the folks at the Triangle Club as it would be to anyone who comes out as queer.
(CJ Higgins is a postdoctoral fellow with the Alexander Grass Humanities Institute at Johns Hopkins University.)

District of Columbia
D.C. Latinx Pride celebrates culture and heritage
Your guide to events throughout June

Organizers with the Latinx History Project have planned a host of events this Pride season with parties, poetry, drag and more.
The festivities begin with the DC Latinx Pride 2026 Kickoff at Crush Dance Bar (2007 14th Street, N.W.) on Friday, June 12 from 6-10 p.m. The party will include a coronation ceremony for the 2026 Royal Court: Ms. DC Latinx Pride Vida Rangel and Mx. DC Latinx Pride Steph Niaupari. RSVP at latinxhistoryproject.org. The event is free, though donations are accepted.
An outdoor event is planned for Sunday, June 14 from 11 a.m.-1 p.m. at Anacostia River Park (1500 Anacostia Dr., S.E.). Cultivating Queer Outdoor Joy is a “peaceful outdoor community event focused on grounding, connection, and queer joy in nature.” The event is free.
A panel discussion is planned for The Festival Center (1640 Columbia Rd., N.W., 2nd floor) on Monday, June 15 from 6-8 p.m. La Plática: The Future of 2 Spirits and Trans Natives will focus upon the “stories, leadership and vision of Two-Spirit, Indigiqueer and Trans Native people.” RSVP to the free event at latinxhistoryproject.org.
A sex-positive poetry workshop, “Hoetry: Writing Erotic Poetry,” is planned for Wednesday, June 17 from 6-8 p.m. at The Festival Center (1640 Columbia Road, N.W.). The event is free.
The workshop So You Wanna Do Drag? is planned for Thursday, June 18 from 5:30-8 p.m. at The Festival Center (1640 Columbia Road, N.W.). Featured guests Ricky Rose and Mari Con Carne will hold a style showcase to discuss the basics of developing a drag persona. RSVP to the free event at latinxhistoryproject.org.
The Latinx History Project is collaborating with Rumba Queer DC to produce an official Latinx Pride Party: Sin Vergüenza. The event is at the multi-level venue, Transmission (1353 H Street, N.E.) on Thursday, June 18 from 7 p.m.-1 a.m. There are dance lessons, vendors and three different music experiences in the sprawling venue. There will also be a drag showcase from 10-11 p.m. The event is 21+ and tickets are available at shotgun.live/en/events/sin-verguenza. Tickets are $15 for entry into the party. Tickets to participate in the dance lesson are $29.98. Participants may choose between a bachata lesson or a salsa lesson from 7-8 p.m.
La Fiesta: Official DC Latinx Pride Party is planned for Friday, June 19 from 10 p.m. – 2 a.m. at Bunker (2001 14th Street, N.W.). Serena Morena from “Drag Race México” and “Drag Race UK vs The World” is slated to headline the 21+ event. Early tickets are available for $15 (plus $0.38 service fee) until June 16. The door cover charge without early tickets is $20. Attendees can also purchase a meet and greet experience with Serena Morena for $30. Tickets are available at latinxhistoryproject.org.
The Latinx History Project plans to march in the Capital Pride Parade on Saturday, June 20 and to have a table at the Capital Pride Festival on Sunday, June 21. Visit latinxhistoryproject.org to register to march alongside LGP in the parade or to staff the table at the festival.
The DC Latinx Pride 2026 Closing Event is scheduled for Friday, June 26 from 6:30-8:30 p.m. at the Mexican Cultural Institute (2829 16th Street, N.W.). The free event is a panel discussion “centering the experiences of immigrants who have lived in Latin America and now call the United States home.”
Visit latinxhistoryproject.org for more information.
District of Columbia
JR.’s hosts meet & greet for mayoral candidate Janeese Lewis George
Event organized by Capital Stonewall Democrats, Queers for Janeese

D.C. mayoral candidate Janeese Lewis George spoke to a crowd of LGBTQ supporters on June 1 at a meet & greet event held at JR.’s on 17th Street in the Dupont Circle neighborhood.
The event, organized by Capital Stonewall Democrats, which has endorsed Lewis George for mayor, with support from a group called Queers for Janeese, was followed by a “get out the vote” canvassing endeavor in which several of those attending the meet & greet visited the homes of nearby residents known to be Lewis George supporters.
The purpose of the canvassing was to remind Lewis George supporters to return their mail-in ballots or go to the polls on June 16 to elect Lewis George as the city’s next mayor, according to Matthew Kavanagh, one of the leaders of Queers for Janeese who attended the meet & greet event at JR.’s.
Local political observers consider Lewis George, a Ward 4 D.C. Council member, and former At-Large D.C. Council member Kenyan McDuffie, to be the two leading candidates in this year’s race for mayor. The two are among seven mayoral candidates competing in the city’s June 16 Democratic primary.
Lewis George told those attending the meet & greet, which was held on the JR.’s outdoor patio, that she has a long record of advocating for and initiating city polices and laws in support of the LGBTQ community. She said large corporate donors were backing her opponents and urged her LGBTQ supporters to help raise funds for her in the remaining days of the campaign.
Among those attending the meet & greet was gay longtime Dupont Circle civic activist Randy Downs who last November opened a nearby eatery called Protest Pizza. “I am queer and I am a Janeese supporter,” Downs told the Blade.
Stevie McCarty, president of Capital Stonewall Democrats, who also spoke at the meet & greet event, said his group would organize events in support of Lewis George in the remaining days of the campaign. Among them, he said, was an LGBTQ bar crawl in which supporters of Lewis George, including the candidate herself, would visit LGBTQ bars to promote her candidacy.

District of Columbia
D.C. kicks off Pride month with flag raising ceremony
Mayor, Council members join LGBTQ activists in 4th annual event

Members of the D.C. Council joined Mayor Muriel Bowser and a crowd of LGBTQ activists and supporters on June 1 for the city’s fourth annual LGBTQ Pride flag raising ceremony held outside the John A. Wilson Building, which serves as the D.C. City Hall.
Since its inception four years ago by Mayor Bowser, the event has served as the official kickoff of D.C. Pride month, which culminates this year with the annual Capital Pride Parade on June 20 and Pride festival on June 21, which takes place on Pennsylvania Avenue, N.W. near the U.S. Capitol.
“As I like to say, we’re celebrating Pride month in the gayest city in the world,” Bowser told a crowd that included city officials and Council members joining her on the front steps of the Wilson Building.
“Fifty-one years of Pride in the future 51st state,” she said, adding, “And both movements are rooted in the same belief – every person deserves to be seen, heard, and fully represented.”
Among those who spoke at the event in addition to Bowser were Japer Bowles, director of the Mayor’s Office of LGBTQ Affairs; D.C. Attorney General Brian Schwalb; and D.C. Council Chair Phil Mendelson (D-At-Large).
“This year is special,” Bowles told the gathering. “It’s special because we celebrate the 20th anniversary of the Mayor’s Office of LGBTQ Affairs,” he said. “For two decades this office has helped make Washington, D.C. one of the most welcoming and affirming cities in the world.”
He added, “We have expanded LGBTQ services across agencies, invested millions of dollars into community organizations, championing culturally competent care and training, supporting LGBTQ supportive businesses and workers and celebrated our history.”
Schwalb said his Office of the D.C. Attorney General continues to safeguard the city’s laws protecting residents against discrimination but expressed concern about “high court” rulings that he said continue to roll back civil rights, voting rights, and human rights.
He said, “We’re seeing cases limiting medical care for transgender youth while at the same time green lighting so-called conversion therapy.” He pointed to cases or policies “excluding transgender girls from participating in sports and excluding story books with LGBTQ characters from our school libraries.”
He said his office is committed to protecting all residents, including LGBTQ residents, from all forms of discrimination. “And that includes the right to be our authentic selves, to freely express our identities and ourselves to be who we are and to love who we love.”
Mendelson, who also expressed strong support for the LGBTQ community and for the upcoming Pride events, said 10 of the Council’s 13 members were attending the Pride flag raising event, including gay Council member Zachary Parker (D-Ward 5).
“I’m just here with gratitude,” Parker told the Washington Blade. “There’s a lot to be grateful for and a lot more to fight for,” he said. “And so, raising this flag is a reminder that our government is here to serve all of our residents regardless of how you identify or who you love.”
Shortly after Mendelson spoke, D.C. Council member Janeese Lewis George (D-Ward 4), who is running for mayor in the city’s June 16 primary, arrived at the event, becoming the 11th Council member to turn out for the event.
Among those also attending the event were Ryan Bos and June Crenshaw, the two top officials of the Capital Pride Alliance, the group that organizes D.C.’s annual LGBTQ Pride events.
Bowser, who is not running for re-election this year and will be stepping down as mayor in January 2027, thanked those attending the Pride flag raising event for playing a role in an all-inclusive city.
“We speak with one clear voice – that D.C. is a welcoming city,” she said in her remarks. “But also, we know that our work has been robust, but it is not done. We fly this flag in front of the John A. Wilson Building because it tells a story,” she said.
“It tells a story of a city that takes care of itself,” she added. “And we take care of each other. We are a city that is diverse and welcoming.”
Serving as the event’s master of ceremony and who introduced Bowles as the first speaker was longtime D.C. drag performer Tara Hoot.
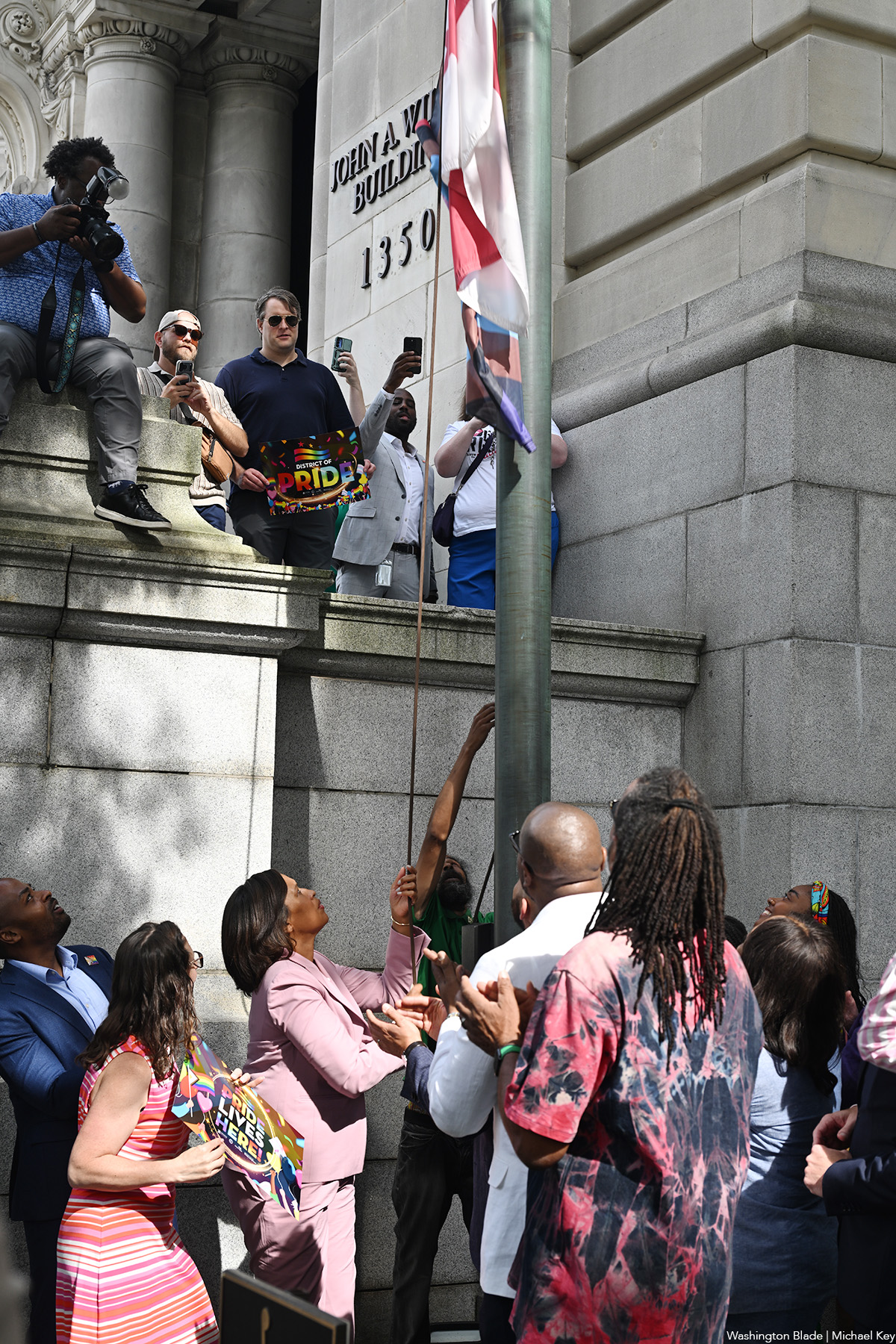
-

 Celebrity News5 days ago
Celebrity News5 days agoOutright International honors Cyndi Lauper at annual NYC gala
-

 Health5 days ago
Health5 days agoAIDS Healthcare Foundation announces 3 million people globally in its care
-

 National5 days ago
National5 days agoResults from key Tuesday primary races
-

 U.S. Military/Pentagon5 days ago
U.S. Military/Pentagon5 days agoFederal appeals court rules White House illegally banned trans troops




















