Health
The transgender surgeon as artist
Calif.-based doctor to appear at Saturday’s Trans Pride event
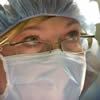
Dr. Marci Bowers is a rarity — she’s one of only two doctors who specializes in gender reassignment surgery who’s also transgender herself. The other (Dr. Christine McGinn) is a protégé of Bowers.
Bowers, who transitioned in the mid-1990s, is the only gynecologist who does gender reassignment surgery. She’ll be at Trans Pride on Saturday (10 a.m. to 5 p.m. at Metropolitan Community Church of Washington) to give the keynote address and took nearly an hour on the phone last week from her practice in San Mateo, Calif., to talk about her life, her work, the practicalities of trans surgical procedures and where trans issues are going. Bowers’ comments have been edited for length and clarity.
Washington Blade: How does a surgeon trained in one area move to another? What kind of training is involved?
Dr. Marci Bowers: Well sometimes people think when you’re a gynecologist all you do is look at female vulvas all day but it’s quite a surgical specialty. There’s extensive surgery experience required before learning the gender reassignment stuff. And after I’d been doing surgery in practice for 13 years or so, once you have a basic framework about handling tissue and bleeding, learning a new skill isn’t as hard as it might seem.
Blade: So if someone does, say, gall bladder surgeries and wants to start doing heart transplants, what’s the process like to move to a whole other part of the body?
Bowers: Traditionally you have to do a fellowship of some kind to do that. You have to go back, reapply as if you’re just out of medical school, do a residency all over again in the new field and go from there. They might give you a little credit on a few things, but you pretty much have to start back at the beginning. It was different for me because there’s no residency or fellowship for doing gender reassignment surgeries and I had a lot of experience surgically so doing an entire residency for me would have been ridiculous and superfluous. It’s really a mentoring process and I learned from Dr. (Stanley) Biber.
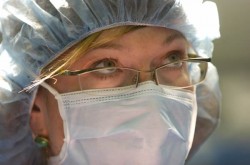
Dr. Marci Bowers says gender reassignment surgery isn’t as traumatic as many fear. Complications, she says, are extremely rare, patients are in the hospital an average of only three nights and most are off pain medication within 48 hours. (Photo courtesy of Bowers)
Blade: Does it give you added credibility to be doing these surgeries but also be transgender yourself?
Bowers: Well, I think that’s really for the consumer to decide that, but I think so. It’s sort of like the hair club for men. Not only am I president, I’m also a customer. Someone who understands what it’s like to be bald. Or like if you’re selling sports cars but you drive a minivan. I know what the consumer is looking for but I think being a gynecologist is the most important. Because it’s a very visual surgery and very artistically based. If someone has a gall bladder out and there are no complications, nobody cares what it looked like but this surgery has such an artistic component, the surgeon’s interpretation is so critical.
Blade: Many trans people say the world is too obsessed with who’s had what done surgically. Do you agree?
Bowers: That’s a crucial point and one that I keep bringing up proactively because obviously people still don’t understand the difference between gender and genitalia. Gender, we know, gets established at a very early age, like by age 4, 5 or 6 and it doesn’t really change very much. This is what transgender people have been saying for years, “This is how I felt since I was 5 years old.” So the question about surgery is really the dumbest question. … I was a woman since I transitioned. Nobody tells you whether you’re male or female. And it isn’t about the surgery, it’s what society says when they meet you at the grocery store or the food counter.
Blade: Trans acceptance seems to be making progress but still seems significantly behind gay and lesbian acceptance. Do you agree with that? Do you think it will continue to improve?
Bowers: Well, yes, I do think we are behind where the lesbian and gay community is in terms of acceptance. Some of that is just the sheer numbers, some of it is it’s still a little bit of a minority sort of thing and somehow it does sort of push people’s buttons in a different way. That’s too bad because if the gay and lesbian community saw the trans community as more supportive, we could make much more progress but sometimes the discrimination we get within the gay and lesbian community is worse than it is with the straight community. It’s like they just don’t get it and it’s very hurtful. There are common threads that run through all kinds of discrimination. We’re fighting the same forces that want to simplify the world and turn back the clock so everything is black and white and keep dragging at the heels of progress.
Blade: What kinds of procedures do you do? All “bottom” stuff or more?
Bowers: Kind of bottom plus. I do a procedure on the females, Chondrolaryngoplasty, which is a shaving of the thyroid cartilage. For some women, it’s a telltale sign in the throat and it was first done by Dr. Biber in the 1970s. It’s also a very delicate procedure that’s not taught anywhere, no ear, nose or throat doctors do it. It’s a very specialized thing.
Blade: And you do both male-to-female and female-to-male gender reassignment procedures?
Bowers: Yes.
Blade: Which are more common? How many do you average in a year?
Bowers: I do about 120 male-to-female surgeries a year. It’s about four-to-one female to male versus male to female.
Blade: Are most people able to orgasm after surgery?
Bowers: It’s different. For female to male, there’s really no impact. With a Metoidioplasty, guys can use it for penetration so that’s the good part there. If anything, it’s enhanced. Plus the fact that they’re testosterone-driven men, the libido tends to accelerate with transition. With male to female, it’s very complicated and about 30 percent of biologically born women aren’t able to orgasm at all anyway. Our patients for the most part are able to. It’s a very high percentile. About 90 percent but the thing you have to realize is that going from male to female for one thing, just hormonally, you tend to go to a lower level of interest just based on reduced testosterone levels. When you’re a woman, you wonder why we leave men in charge of so much. It’s so dominated by sexual thoughts. Sometimes I think, “Wow, what was I thinking about all those years? There’s so much more to do.” I say that sort of tongue in check. And the feelings are a big different. Maybe like going from the oboe to the banjo.
Cannabis Culture
LGBTQ people, weed, and mental health: what you need to know
Community uses marijuana at much higher rates than general population

Uncloseted Media published this story on May 7.
By SPENCER MACNAUGHTON | In 2025, the global cannabis market size was valued at nearly $103 billion. By 2034, that number is expected to explode by roughly 1,400 percent to more than $1.43 trillion.
In short, as an increasing number of countries legalize marijuana use, everyone is starting to consume a lot more weed. And LGBTQ people tend to use cannabis at much higher rates than the general population. One study found that 55 percent of lesbian and 45 percent of gay young adults use marijuana, compared to about 33 percent and 37 percent, respectively, of their straight counterparts.
As LGBTQ people face a mental health crisis, the mainstream stereotypes that depict weed as an antidote for anxiety, panic and depression aren’t painting the full picture. And that could be exacerbating the mental health struggles so many queer people, and especially youth, face.
Here’s what the research demonstrates about marijuana and its effects on mental health:
- Multiple studies suggest a link between marijuana use and an increased risk of mental health disorders, including schizophrenia, depression and anxiety in individuals who are genetically predisposed.
- One study found that daily marijuana use, especially among younger people, makes some individuals seven times more likely to develop psychosis.
The increase in higher-potency strains of marijuana could pose unknown risks. In 1995, the average content of Tetrahydrocannabinol (THC) in confiscated marijuana was less than 4 percent. In 2022, it was more than 16 percent. Researchers don’t know the full extent of the impact that these higher concentrations can have on mental health and especially on younger people whose brains are still developing.
- A systematic review of studies published between 2013 and 2025 found damning results for the mental health of young cannabis users:
They were 51 percent more likely to experience depression, 58 percent more likely to experience anxiety, between 50 and 65 percent more likely to experience suicidal ideation and 80 to 87 percent more likely to have attempted suicide.
- While the above stats paint a grim picture, there is also some research that suggests benefits of cannabis use:
- A 2025 systematic review found that “medicinal” weed showed some efficacy in relieving withdrawal symptoms of opioid use disorder. THC use has been associated with improvement of post-traumatic stress disorder symptoms, bipolar symptoms and sleep quality.
- Other studies found that THC administered in a controlled setting was associated with a decrease of symptoms and adverse effects for a range of mental health disorders, including schizophrenia, psychotic symptoms, and anorexia nervosa.
Beyond what we pulled from academia, there is an astounding lack of information about the interplay between weed and mental health. As we dive deeper into Mental Health Awareness Month, I hope advocacy organizations, influencers and news outlets ramp up their coverage of this important topic that affects the countless LGBTQ weed smokers, many of whom are already struggling.
Health
UPDATED: Trans-led HIV clinic in Portsmouth struggles amid funding cuts
As states across the U.S. cut funding for HIV care this small clinic in Va, is still fighting

Two years ago, Nyonna Byers, a transgender woman from Portsmouth, Va., founded Ending Transmission of Sexual Infections (ETSI) Health Clinic to support a community she saw struggling with rising HIV rates. Now, as costs continue to climb and funding for HIV healthcare initiatives is being cut across the United States, Byers says her transgender identity has made it harder to secure the financial support her clinic needs to survive.
Portsmouth, with just under 100,000 people, is right across the Elizabeth River from Norfolk.
“We’re an HIV-led organization here in Portsmouth, providing services throughout the Hampton Roads area,” Byers told the Blade. “As a trans-led organization—with me as the founder and executive director—I’ve received a lot of rejection when it comes to funding. That’s one of the main reasons why we’re struggling to keep the clinic open. Without funding, we can’t provide HIV treatment or care, and then we’re just a theoretical organization—we can’t be impactful in the community we serve.”
She said the data clearly shows a need for increased investment in HIV care in Portsmouth, but the response from leadership has not matched the urgency of the crisis.
“Portsmouth is one of the smallest cities with one of the highest HIV rates, and there are very few HIV-led organizations or clinics here. The need is urgent, but the response doesn’t match it. We’re doing the work on the ground, but we’re not getting the support to sustain it. That disconnect is what’s hurting people the most.”
That need, Byers explained, continues to grow as ETSI struggles to meet the financial demands of the life-saving work it provides.
Portsmouth has one of the highest HIV prevalence rates in Virginia, with roughly 736.9 cases per 100,000 people—a rate that exceeds both state and national averages.
“Leaders like the mayor and city council don’t focus on public health or social health. They focus more on development—building the city up physically—rather than investing in the health of the people. I’ve applied for funding multiple times and been denied. Every time I’ve asked for resources, I’ve been turned away.”
When asked why, Byers said the answer felt clear to her.
“I honestly believe I was denied funding because I’m trans. I told the mayor I was going to go public with it, because it’s not fair. We’re on the ground doing the work to end HIV, and we’re still not getting the support we need. That’s not just frustrating—it’s harmful.”
While she said local support has been lacking, Byers noted that the state has stepped in—though the funding still falls short of what is needed to sustain the clinic long term.
ETSI Health Clinic was included as a recipient of funding in the Virginia 2027–2028 Senate budget, receiving $50,000 per year from the Virginia General Fund. Byers specifically credited State Sen. Lillie Louise Lucas with helping secure that funding, which she said did not come from city leadership.
Byers shared that she has given up a lot to keep ETSI afloat, but the costs just keep coming.
“I’ve worked a lot of contracts—jobs paying $30 to $40 an hour—and poured that money into my clinic. But the downside is that I’m struggling personally. I’ve lost cars, I’ve lost a house—I’ve lost a lot to keep this clinic going. This work has cost me almost everything.”

She added that the impact of federal policy shifts is also being felt locally. As the Trump-Vance administration continues to roll back what it has described as unnecessary “DEI” spending, Byers said those decisions are affecting clinics like hers.
There was a time when the clinic was able to receive funding from Sentara Cares, the philanthropic program of Sentara Health, a not-for-profit healthcare system based in Virginia and North Carolina, but now they can’t.
“We had funding from Sentara Cares for three years, and it helped keep us going. Then when DEI initiatives started getting rolled back, that funding stopped. I was told directly that because of federal policy changes, they couldn’t fund the clinic. I broke down during that meeting, because it felt like they were really saying they couldn’t support us because of who we are.”
That lack of funding is compounded by broader gaps in healthcare access in the region. Portsmouth—the ninth most populous city in Virginia—does not have a hospital.
“There’s very limited access to care in Portsmouth. We don’t even have a hospital—people have to be transported to Norfolk. We’ve had high rates of syphilis, and the health department is only open a few days a week. A lot of people don’t trust it, and that leaves entire communities without care.”
Byers made it clear that this is more than a passion project for her—it is her life’s calling, and she would do nearly anything to keep it going.
“To be honest, I would go back to sex work before I let my clinic close. This is something I built from the ground up. I built this clinic with money I earned myself. I’m not going to let it disappear without a fight.”
She also pointed to gaps in education and outreach, which she says exacerbate HIV rates despite the availability of preventive measures.
“There’s almost no marketing or education about PrEP in the Hampton Roads area. If you go to places like D.C. or Atlanta, you see billboards and campaigns—but here, you don’t see anything. If people don’t see it, they don’t know about it. That lack of awareness is putting people at risk.”
It is also a deeply personal fight, she explained.
“I’ve lost friends to HIV. People say you can’t die from HIV anymore, but you can if you’re not in care. I’ve seen it firsthand, and that’s what motivates me to keep going. HIV doesn’t have to be a death sentence—but without support, it can become one.”
The Blade reached out to Portsmouth Mayor Shannon E. Glover for comment.
Glover disputed Byers’ claims that her clinic was treated unfairly, including her allegation that her transgender identity played a role in funding decisions.
“There’s no issue with Miss—with her and her organization. We have been in discussion, and quite frankly, the claims that she made as it relates to ‘we’re not treating her equitably and fairly because of her [being] transgender’ that is totally untrue,” Glover told the Blade via phone call. “I’ve talked to Miss Nyonna on a number of occasions, and that is categorically not true.”
Glover added that the city provides funding to various organizations and said he had directed Byers to seek support elsewhere.
“So I’m not understanding what her issues are,” he said. “But in any event, you know, we have funding that we provide to organizations. I’ve recommended other organizations to her. I’ve recommended that she go to the state where they have more flexibility with their budget and they could help her. So that’s what I’m prepared to tell you today. I’m not going to answer any questions. I just wanted to respond that her claim that we are mistreating her, not treating her fair, is totally untrue.”
To donate to ETSI, visit their donation page at ESTIhcvas.org/donate
Health
Housewives head to Capitol Hill to promote PrEP coverage
Bravo’s Real Housewives stars to lobby lawmakers for expanded PrEP access.

Stars from Bravo’s hit franchise “The Real Housewives” are heading to Capitol Hill next week to advocate for expanded access to HIV prevention and treatment.
On March 18, several well-known cast members — including NeNe Leakes, Phaedra Parks, Candiace Dillard Bassett, Erika Jayne, Luann de Lesseps, Melissa Gorga, and Marysol Patton — will travel to D.C. to participate in an advocacy event aimed at increasing awareness and coverage for pre-exposure prophylaxis, commonly known as PrEP.
The event, dubbed “Housewives on the Hill,” is being organized by MISTR, the nation’s largest telehealth platform focused on sexual health. The group’s founder and CEO, Tristan Schukraft, will join the reality television stars as they meet with lawmakers and legislative staff to discuss the importance of maintaining and expanding access to HIV prevention tools.
PrEP is a medication regimen that can, if taken properly, reduce the risk of contracting HIV through sex by up to 99 percent according to public health officials. Advocates say wider access to the medication — including through insurance coverage and telehealth services — is critical to reducing new HIV infections across the United States.
During their day on Capitol Hill, the Housewives are expected to meet with members of Congress and participate in conversations about federal policies affecting HIV prevention and treatment. Organizers say the reality stars will also share personal reflections about the continued impact of HIV on communities across the country and the importance of keeping prevention resources accessible.
The “Housewives on the Hill” event aims to use the cultural influence of the Bravo stars to spotlight HIV prevention efforts and encourage lawmakers to protect and expand access to lifesaving medication and treatment options. Organizers say the goal is simple: ensure that more Americans can access the tools they need to prevent HIV and maintain their sexual health.



















