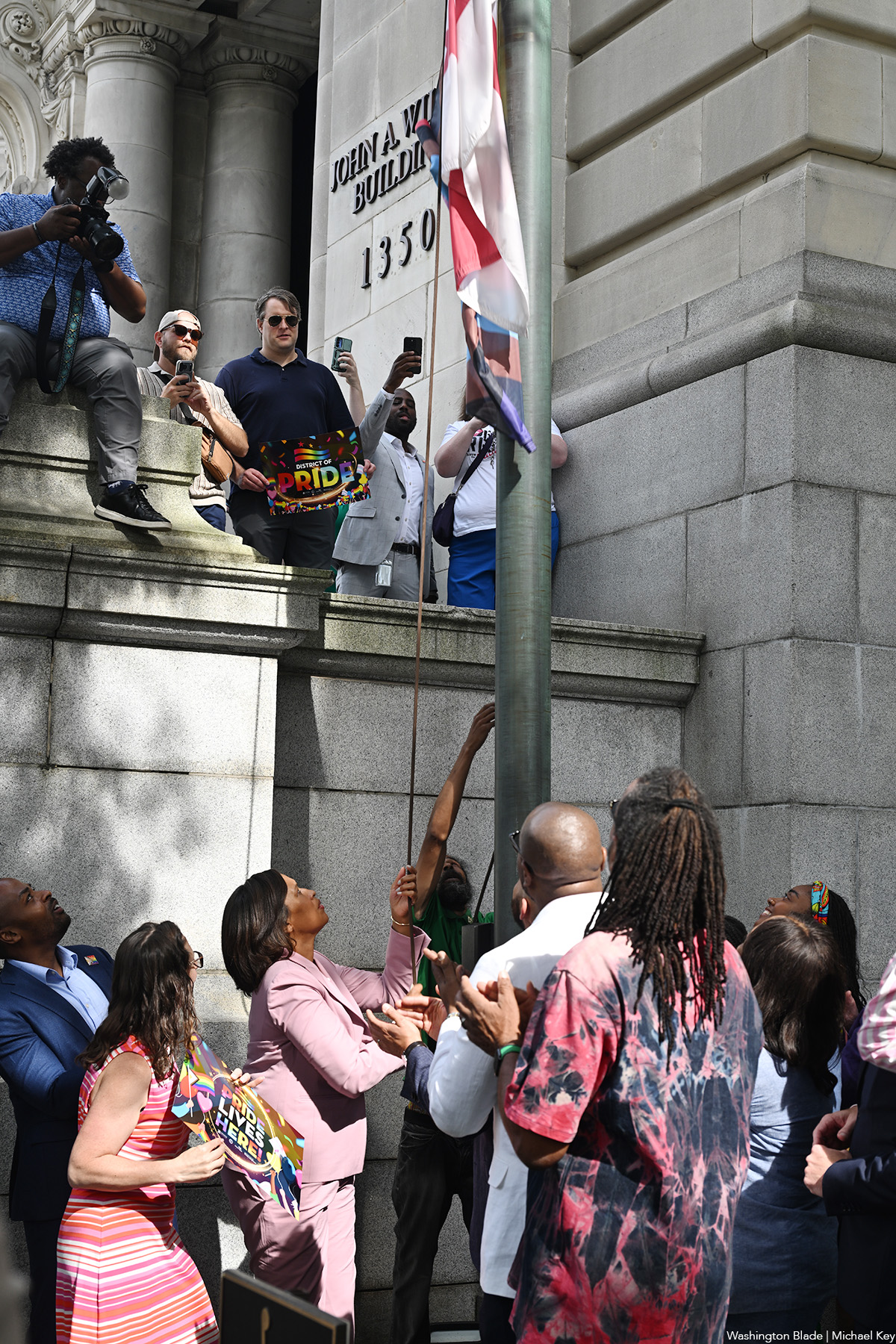District of Columbia
New complaint form to help D.C. LGBTQ seniors facing discrimination
Office of Human Rights steps up protections for those in long-term care

The D.C. Office of Human Rights (OHR) announced on July 22 that it is launching new “user-friendly” intake forms designed to facilitate and simplify the filing of discrimination complaints by seniors, including LGBTQ seniors, who encounter discrimination in long-term care facilities such as nursing homes.
“The forms simplify the complaint filing process, making it easier for residents to better access support and understand their rights” at long term care facilities, according to a statement released by OHR. The statement provides a link to access the new intake forms online.
“This initiative is part of OHR’s Care for Seniors program, which supports LGBTQ seniors and seniors living with HIV facing discrimination in such facilities,” the statement continues. “The form addresses concerns related to sexual orientation, gender identity or expression, HIV status, and other prohibited bases of discrimination, streamlining the reporting process and enabling seniors to file claims directly through OHR’s website,” it states.
In addition to the improved intake form for seniors filing discrimination complaints, the OHR announcement says it is also releasing new forms for filing complaints under the D.C. Universal Paid Family Leave Amendment Act, which requires employers in the city to provide 12 weeks of paid leave benefits for parental, family, or medical reasons to eligible employees.
“The form allows individuals to file complaints if they believe their employer has interfered with their right to these benefits or retaliated against them for requesting, applying for, or using paid leave” in violation of the law in question, according to the statement.
OHR officials have pointed out that D.C. stepped up its protections for LGBTQ seniors through the passage by the D.C. Council of the Care for LGBTQ Seniors and Seniors with HIV Amendment Act of 2020. Among other things, the law calls for OHR certified trainers to “provide specialized information for staff in long-term care facilities, specifically tailored to meet the unique needs of LGBTQ+ seniors and seniors with HIV in long-term care facilities,” OHR states in its website.
“We prioritize safeguarding the new rights and legal protections outlined in the Act, which includes a posted notice of ‘Non-Discrimination’ aiming to ensure that participating facilities actively contribute to creating secure and inclusive environments for all residents,” the OHR website statement concludes.
The questionnaire and complaint form for LGBTQ seniors facing discrimination in long-term care facilities can be accessed at ohr.dc.gov.
District of Columbia
D.C. Latinx Pride celebrates culture and heritage
Your guide to events throughout June

Organizers with the Latinx History Project have planned a host of events this Pride season with parties, poetry, drag and more.
The festivities begin with the DC Latinx Pride 2026 Kickoff at Crush Dance Bar (2007 14th Street, N.W.) on Friday, June 12 from 6-10 p.m. The party will include a coronation ceremony for the 2026 Royal Court: Ms. DC Latinx Pride Vida Rangel and Mx. DC Latinx Pride Steph Niaupari. RSVP at latinxhistoryproject.org. The event is free, though donations are accepted.
An outdoor event is planned for Sunday, June 14 from 11 a.m.-1 p.m. at Anacostia River Park (1500 Anacostia Dr., S.E.). Cultivating Queer Outdoor Joy is a “peaceful outdoor community event focused on grounding, connection, and queer joy in nature.” The event is free.
A panel discussion is planned for The Festival Center (1640 Columbia Rd., N.W., 2nd floor) on Monday, June 15 from 6-8 p.m. La Plática: The Future of 2 Spirits and Trans Natives will focus upon the “stories, leadership and vision of Two-Spirit, Indigiqueer and Trans Native people.” RSVP to the free event at latinxhistoryproject.org.
A sex-positive poetry workshop, “Hoetry: Writing Erotic Poetry,” is planned for Wednesday, June 17 from 6-8 p.m. at The Festival Center (1640 Columbia Road, N.W.). The event is free.
The workshop So You Wanna Do Drag? is planned for Thursday, June 18 from 5:30-8 p.m. at The Festival Center (1640 Columbia Road, N.W.). Featured guests Ricky Rose and Mari Con Carne will hold a style showcase to discuss the basics of developing a drag persona. RSVP to the free event at latinxhistoryproject.org.
The Latinx History Project is collaborating with Rumba Queer DC to produce an official Latinx Pride Party: Sin Vergüenza. The event is at the multi-level venue, Transmission (1353 H Street, N.E.) on Thursday, June 18 from 7 p.m.-1 a.m. There are dance lessons, vendors and three different music experiences in the sprawling venue. There will also be a drag showcase from 10-11 p.m. The event is 21+ and tickets are available at shotgun.live/en/events/sin-verguenza. Tickets are $15 for entry into the party. Tickets to participate in the dance lesson are $29.98. Participants may choose between a bachata lesson or a salsa lesson from 7-8 p.m.
La Fiesta: Official DC Latinx Pride Party is planned for Friday, June 19 from 10 p.m. – 2 a.m. at Bunker (2001 14th Street, N.W.). Serena Morena from “Drag Race México” and “Drag Race UK vs The World” is slated to headline the 21+ event. Early tickets are available for $15 (plus $0.38 service fee) until June 16. The door cover charge without early tickets is $20. Attendees can also purchase a meet and greet experience with Serena Morena for $30. Tickets are available at latinxhistoryproject.org.
The Latinx History Project plans to march in the Capital Pride Parade on Saturday, June 20 and to have a table at the Capital Pride Festival on Sunday, June 21. Visit latinxhistoryproject.org to register to march alongside LGP in the parade or to staff the table at the festival.
The DC Latinx Pride 2026 Closing Event is scheduled for Friday, June 26 from 6:30-8:30 p.m. at the Mexican Cultural Institute (2829 16th Street, N.W.). The free event is a panel discussion “centering the experiences of immigrants who have lived in Latin America and now call the United States home.”
Visit latinxhistoryproject.org for more information.
District of Columbia
JR.’s hosts meet & greet for mayoral candidate Janeese Lewis George
Event organized by Capital Stonewall Democrats, Queers for Janeese

D.C. mayoral candidate Janeese Lewis George spoke to a crowd of LGBTQ supporters on June 1 at a meet & greet event held at JR.’s on 17th Street in the Dupont Circle neighborhood.
The event, organized by Capital Stonewall Democrats, which has endorsed Lewis George for mayor, with support from a group called Queers for Janeese, was followed by a “get out the vote” canvassing endeavor in which several of those attending the meet & greet visited the homes of nearby residents known to be Lewis George supporters.
The purpose of the canvassing was to remind Lewis George supporters to return their mail-in ballots or go to the polls on June 16 to elect Lewis George as the city’s next mayor, according to Matthew Kavanagh, one of the leaders of Queers for Janeese who attended the meet & greet event at JR.’s.
Local political observers consider Lewis George, a Ward 4 D.C. Council member, and former At-Large D.C. Council member Kenyan McDuffie, to be the two leading candidates in this year’s race for mayor. The two are among seven mayoral candidates competing in the city’s June 16 Democratic primary.
Lewis George told those attending the meet & greet, which was held on the JR.’s outdoor patio, that she has a long record of advocating for and initiating city polices and laws in support of the LGBTQ community. She said large corporate donors were backing her opponents and urged her LGBTQ supporters to help raise funds for her in the remaining days of the campaign.
Among those attending the meet & greet was gay longtime Dupont Circle civic activist Randy Downs who last November opened a nearby eatery called Protest Pizza. “I am queer and I am a Janeese supporter,” Downs told the Blade.
Stevie McCarty, president of Capital Stonewall Democrats, who also spoke at the meet & greet event, said his group would organize events in support of Lewis George in the remaining days of the campaign. Among them, he said, was an LGBTQ bar crawl in which supporters of Lewis George, including the candidate herself, would visit LGBTQ bars to promote her candidacy.

District of Columbia
D.C. kicks off Pride month with flag raising ceremony
Mayor, Council members join LGBTQ activists in 4th annual event

Members of the D.C. Council joined Mayor Muriel Bowser and a crowd of LGBTQ activists and supporters on June 1 for the city’s fourth annual LGBTQ Pride flag raising ceremony held outside the John A. Wilson Building, which serves as the D.C. City Hall.
Since its inception four years ago by Mayor Bowser, the event has served as the official kickoff of D.C. Pride month, which culminates this year with the annual Capital Pride Parade on June 20 and Pride festival on June 21, which takes place on Pennsylvania Avenue, N.W. near the U.S. Capitol.
“As I like to say, we’re celebrating Pride month in the gayest city in the world,” Bowser told a crowd that included city officials and Council members joining her on the front steps of the Wilson Building.
“Fifty-one years of Pride in the future 51st state,” she said, adding, “And both movements are rooted in the same belief – every person deserves to be seen, heard, and fully represented.”
Among those who spoke at the event in addition to Bowser were Japer Bowles, director of the Mayor’s Office of LGBTQ Affairs; D.C. Attorney General Brian Schwalb; and D.C. Council Chair Phil Mendelson (D-At-Large).
“This year is special,” Bowles told the gathering. “It’s special because we celebrate the 20th anniversary of the Mayor’s Office of LGBTQ Affairs,” he said. “For two decades this office has helped make Washington, D.C. one of the most welcoming and affirming cities in the world.”
He added, “We have expanded LGBTQ services across agencies, invested millions of dollars into community organizations, championing culturally competent care and training, supporting LGBTQ supportive businesses and workers and celebrated our history.”
Schwalb said his Office of the D.C. Attorney General continues to safeguard the city’s laws protecting residents against discrimination but expressed concern about “high court” rulings that he said continue to roll back civil rights, voting rights, and human rights.
He said, “We’re seeing cases limiting medical care for transgender youth while at the same time green lighting so-called conversion therapy.” He pointed to cases or policies “excluding transgender girls from participating in sports and excluding story books with LGBTQ characters from our school libraries.”
He said his office is committed to protecting all residents, including LGBTQ residents, from all forms of discrimination. “And that includes the right to be our authentic selves, to freely express our identities and ourselves to be who we are and to love who we love.”
Mendelson, who also expressed strong support for the LGBTQ community and for the upcoming Pride events, said 10 of the Council’s 13 members were attending the Pride flag raising event, including gay Council member Zachary Parker (D-Ward 5).
“I’m just here with gratitude,” Parker told the Washington Blade. “There’s a lot to be grateful for and a lot more to fight for,” he said. “And so, raising this flag is a reminder that our government is here to serve all of our residents regardless of how you identify or who you love.”
Shortly after Mendelson spoke, D.C. Council member Janeese Lewis George (D-Ward 4), who is running for mayor in the city’s June 16 primary, arrived at the event, becoming the 11th Council member to turn out for the event.
Among those also attending the event were Ryan Bos and June Crenshaw, the two top officials of the Capital Pride Alliance, the group that organizes D.C.’s annual LGBTQ Pride events.
Bowser, who is not running for re-election this year and will be stepping down as mayor in January 2027, thanked those attending the Pride flag raising event for playing a role in an all-inclusive city.
“We speak with one clear voice – that D.C. is a welcoming city,” she said in her remarks. “But also, we know that our work has been robust, but it is not done. We fly this flag in front of the John A. Wilson Building because it tells a story,” she said.
“It tells a story of a city that takes care of itself,” she added. “And we take care of each other. We are a city that is diverse and welcoming.”
Serving as the event’s master of ceremony and who introduced Bowles as the first speaker was longtime D.C. drag performer Tara Hoot.